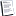
Auto-fusion in a virgin spine or in a post-ADR spine seems to be considered a good result. Stable and immobile is often the goal that represents a successful surgery.
These beak-like, bridging or 'claw' osteophytes do represent auto-fusion... the body is trying to immobilize the segment. They indicate how far down the degenerative process these segements are. When too far advanced, it may be best to let it go... not try to reverse... or remobilize.
Relative to ADR, as the osteophytes grow larger and larger, there are serious bone quality issues. The vertebral bodies are hard around the outside, where there is hard, cortical bone. They are soft in the middle, where there is soft cancellous bone.
As the osteophytes brow larger, the soft cancellous bone in the center of the vertebral body moves outward as the margins of the vertebral body moves outward with the osteophyte... either anterior as in nn's case, or posterior as in my case. If you lop off the osteophyte, if you are removing the bulk of the cortical bone that should have been supporting the prosthesis, leaving the softer bone that has moved outward, following the osteophyte; the risk of subsidence is substantially increased.
Because I'm concerned about this for my case, I've been discussing it extensively with the docs for years. Bertagnoli has been successful in pushing the limits as he understands more and more about what can and cannot be done. What may have been considered a contra-indication years ago, may not be a more ordinary case (for someone with experience with these further advanced cases.)
IMHO, bone wax is taking on too much importance in this discussion. There are structural issues... there is the issue of remobilizing an already immobilized segment... there is the issue of appropriateness of ADR with such advanced degeneration and modic changes... bone wax is just a tool that reduces the risk of undesired bone growth. I've seen some of the studies that discuss the risks associated with bone wax. It does not surprise me to hear that horror stories abound as technologies are misused or abused. I'm sure that the risks are very real and I'm also sure that some doctors will know what they are doing to appropriately manage the risks and proper application of a technology.
I'm about to spend some weeks in Germany and will spend time with both Zeegers and Bertagnoli... I'll post what I learn.
Mark
|